International Journal of Sexual and Reproductive Health Care
Juvenile granulosa cell ovarian tumors: Report of a case
Department of Gynecology and Obstetrics, EHS Nouar Fadela, Oran, Algeria
Author and article information
Cite this as
Sihem D, Yacine BM (2024) Juvenile granulosa cell ovarian tumors: Report of a case. Int J Sex Reprod Health Care. 2024; 7(1): 19-22. Available from: 10.17352/ijsrhc.000044
Copyright License
© 2024 Sihem D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Juvenile granulosa tumors of the ovary are rare tumors.
We report the case of juvenile granulosa cell tumor affecting a 33-year-old woman operated on for pain pelvic, the tumor was located in the left ovary with moderate ascites.
The purpose of this work is to present the anatomoclinical and radiological characteristics of this tumor in order to allow an early diagnosis and to improve its prognosis, to establish a therapeutic chronology for this tumor.
Different prognostic factors for ovarian granulosa cell tumor are being studied; the treatment is surgical.
Granulosa tumors were described for the first time in 1855 by Rokitansky [1], due to their appearance similar to that of granulosa cells in ovarian follicles.
The natural history is only reported in the literature through short series, in the 19th century, it was Vonkahladen, in 1895, who individualized granulosa cell tumors, sarcomas, and carcinomas.
In 1914 Vonwerdt published his first series of six cases and the name granulosa tumor was adopted.
In 1977, Scully, et al. subdivided juvenile and adult granulosa tumor [2].
They arise from the parenchyma and the sexual cord of the ovary, they represent 0.6% - 3% of all ovarian tumors, and 5% of malignant ovarian tumors, they are the most common tumors stromal [3], we distinguish two types: adult granulosa tumor (TGA) between 40 and 70 years, the most common, and juvenile granulosa tumor (TGJ) younger age [4].
The latter represent characteristics different from other tumors such as the morphological, histological signs, a higher risk of recurrence [1,5,6].
Clinically the tumor manifests itself as a tumor syndrome with painful abdominal distension, an endocrine syndrome linked to hyperestrogen giving pseudo-precocious puberty in juvenile forms [7].
Juvenile granulosa tumors generally have a very good prognosis: 92% 5-year survival [8]. Poor prognostic factors are: large size, ascites and capsular rupture [8].
Patient consent is obtained before publication.
Case report
K.F woman aged 33 years, mother of two children, originally from Tiaret and residing in that, with no particular medical or surgical history, who presented to the department for paroxysmal pelvic pain accentuated on the left, clinical examination revealed good general condition, blood pressure 12/06, abdominal palpation revealed accentuated sensitivity on the left.
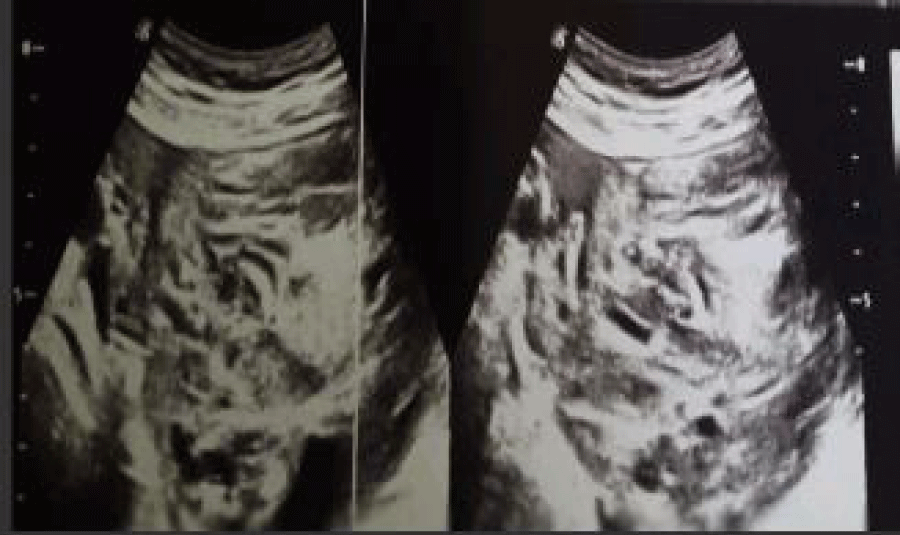
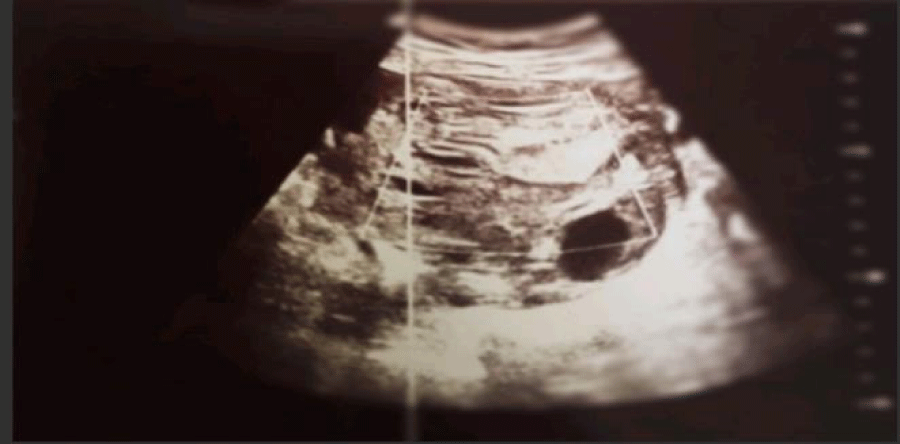
Ultrasound (Figure 1a) revealed a heterogeneous left lateral uterine mass measuring 10 cm in long axis, with a dual tissue and fluid component (Figure 1b) of suspicious appearance with moderate ascites.
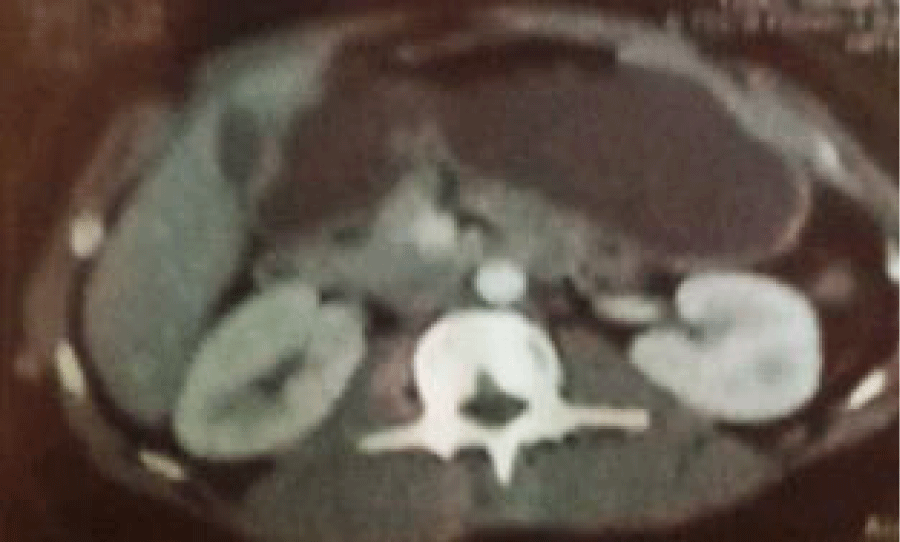
The scan of abdominopelvic (Figure 2) revealed a large, well-circumscribed median pelvic mass measuring 80/110 mm for its longest axes, extending in height to approximately 85 mm, enhancing after injection of the contrast product and heterogeneously delimiting fluid areas in places, calcification coming into contact with the uterine font with respect for the fatty interface of separation.
Homogeneous free ascites of average peri-lesional abundance with pelvic filling, absence of adenomegaly.
The biological assessment is unremarkable.
Tumor markers: CA 125: 62.84 U/ml
A midline subumbilical laparotomy was carried out, revealing a large tumor located on the left measuring approximately 08/12 cm, solid cystic, grayish white with necrotic and hemorrhagic changes, ascites of medium abundance of citrine yellow color.
The patient initially underwent an enucleation cystectomy with sampling of ascitic fluid.
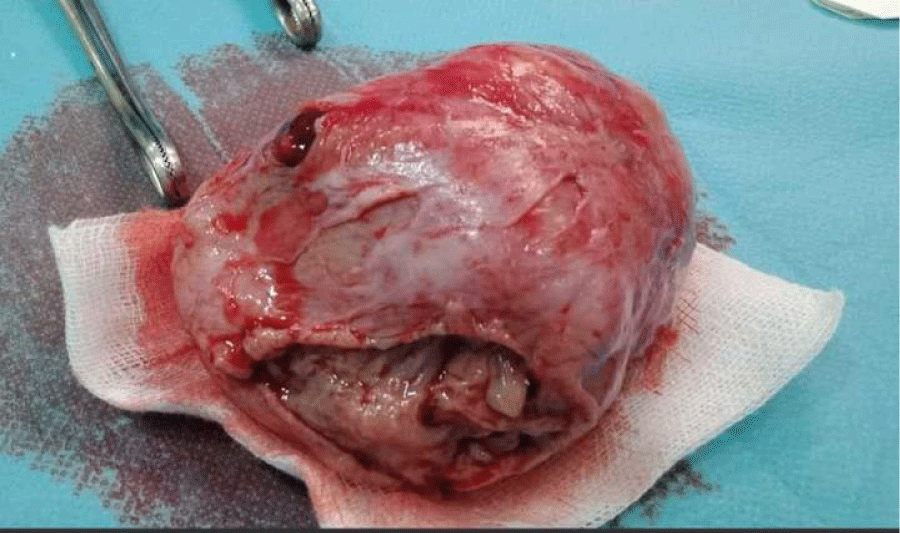
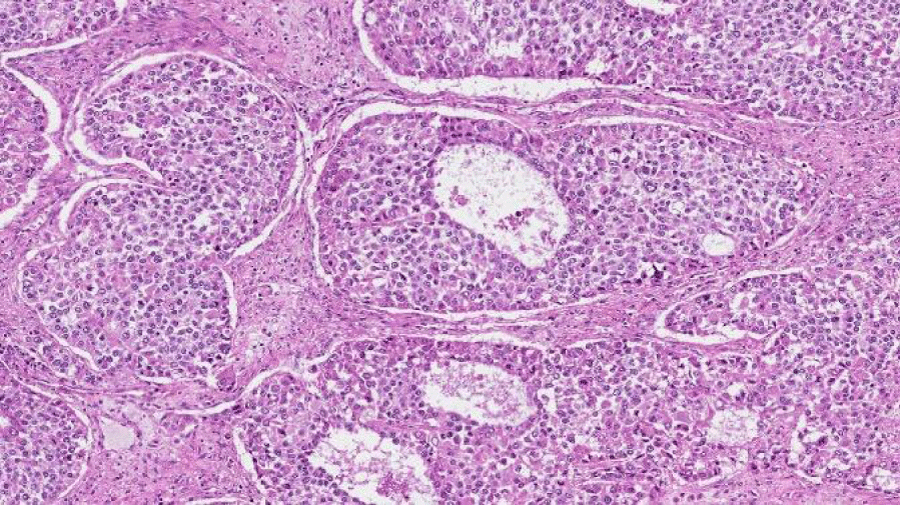
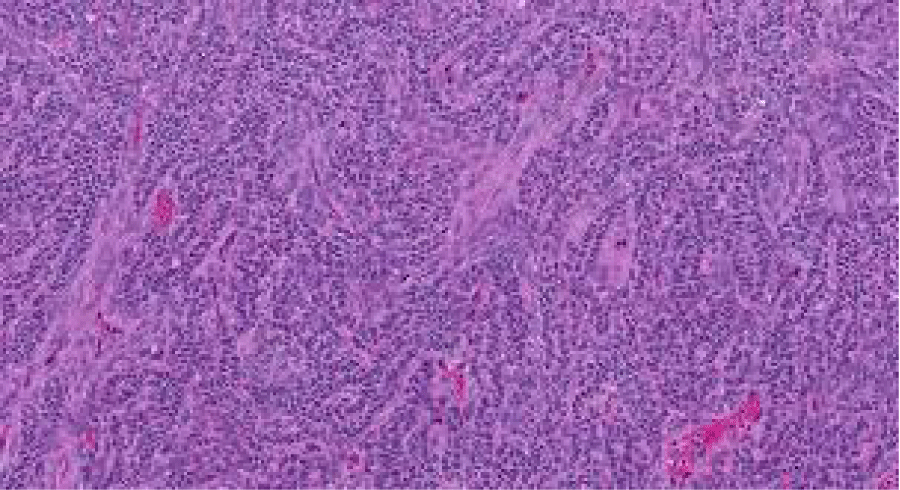
The pathological study of the surgical specimen (Figure 3) suggested the diagnosis of ovarian granulosa cell tumor.
Cytobacteriological examination of the sample fluid: absence of malignant cells.
Different Anatomopathological Types of Ovarian Granulosa Cell Tumors (Figures 4,5).
Discussion
An ovarian tumor can reach a size important before causing abdominopelvic symptoms, which can be very varied and are never specific.
The clinical examination must be complete, including an examination abdominal, palpation of the lymph node areas and touching pelvic (vaginal and rectal). Abdominopelvic ultrasound suprapubic and endovaginally demonstrate an ovarian tumor with malignancy criteria.
The diagnostic assessment will be completed if necessary, by a pelvic MRI and immunohistochemistry CA-125, CA-199, ACE, HCG, AFP.
The positive diagnosis of certainly is based on histological results which can only be obtained by surgical exploration: laparotomy or laparoscopy.
- Treatment of rare ovarian tumors currently rests essentially on surgery whose modalities (conservative or not) depending on histological type, the age of the patient and the stage of the disease.
The chemotherapy protocols are different, chosen according to the histological type.
Principles of surgery before chemotherapy
- The initial surgical procedure is essential in the event of rare ovarian tumors since it allows the diagnosis, assessment extension of the disease and the first therapeutic act. It is not no different technically from that of other malignant tumors ovaries.In the event of a suspicious ovarian tumor discovered in a young woman of childbearing age, it is important that the surgeon considers the diagnosis of tumor epithelial and have a certain amount taken before surgery number of blood markers that can guide the diagnostic ; in the hypothesis of a germ cell tumor: chorionic gonadotropin Hormone (hCG), alpha-fetoprotein; in the hypothesis of a tumor of the sex cords: Anti-Mullerian Hormone (AMH), inhibin a complete exploration of pelvis and the entire abdominal cavity, peritoneal washing and/or a sample of any ascites present during opening the abdomen, peritoneal biopsies systematic procedures including
- The omentum and sampling of any suspicious element.
Principles of secondary surgery after Chemotherapy
Remain subject to discussion, poses differently depending on the histological types studied and has few indications for patients in complete response. The indications seem more clearly established for germ cell tumors than they can be for sex cord tumors, clear cell carcinomas or mucinous tumors.
Granulosa tumors are rare ovarian neoplasias, 70% of malignant tumors in the group of mesenchymal and sex cord tumors [9] and 5% among malignant ovarian tumors [3].
Menopausal status, gravidity and parity have no influence on the appearance of granolosa tumors.
The juvenile form is far less common, it represents only 5% of granulosa tumors [1], juvenile granulosa cell tumor classically occurs in women young people aged 30 years or in the pre-pubertal period [2,10].
It represents 10% of the etiologies of precocious puberty [2], a picture of hyperestrogen with pseudo precocious puberty is revealing in 70% of cases, much more rarely signs of virilization can appear linked to hyperandrogenism [2,3,10,11].
The ultrasound and tomographic appearance of TCGJ is that of an extensive multi-cystic ovarian tumor often with hemorrhagic changes, calcifications and peritoneal nodules are rarely reported [2,6], magnetic resonance imaging MRI visualizes a complex pelvic mass, the hemorrhagic character of cyst (hyper signal on weighted T1) is quite suggestive [4,6].
Biologically: Serum and urinary levels of eostradiol generally increase, plasma levels of gonadotropins (FSH, LH) are reduced [2,11,12], in virilizing forms, testosterone and delta 4 androstenedione levels are increased [11].
TCGJ often presents as a large cystic, multilocular tumor with citrine yellow or gray tissue contingent, pure solid or unilocular cystic tumors are reported, extensive hemorrhagic and necrotic changes are common suggesting a high degree of malignancy [4,6,11], the diagnosis is histological revealing a diffuse or macrofollicular proliferation of luteinized medium cells, mitotic activity is generally absent in the adult form, and evident in the juvenile form our patient was a young adult, she presented with pelvic pain accentuated on the left, abdominal palpation revealed accentuated sensitivity on the left an ultrasound scan showed a 10 cm damaged ovarian tumor, with a heterogeneous component, medium-volume ascites; The patient initially underwent an enucleation cystectomy with ascitic fluid sampling.
The pathological study of the surgical specimen (Figure 3) suggested the diagnosis of ovarian granulosa cell tumor.
Cytobacteriological examination of the sample fluid: absence of malignant cells.
A laparotomy is indicated for her to complete the surgical procedure, a total hysterectomy with bilateral adnexectomy, pelvic lymph node dissection and omentectoma.
Pathological result: Absence of tumor remains in the left appendix. The hysterectomy specimen with the right appendix, the omentectomy specimen and the appendix show no tumor infiltration. The three lymph nodes found in the right dissection as well as the four others found in the left dissection are all reactive, without tumor infiltration.
Step Pt1apN0pMx.
The differential diagnosis arises mainly with undifferentiated carcinomas, adenocarcinomas, carcinoid tumors and endometrioid carcinoma.
The treatment of these tumors is surgical, conservative in young women wishing to become pregnant and presenting with early stage 1a [11,12]. Advanced stage and early stage tumors.
Tumors presenting poor prognostic factors (large size, ascites, histological factor indicating a high risk of recurrence), and recurrent forms requiring polychemotherapy.
Our patient was stage 1a, she benefited from radical surgical treatment given her congestion with moderate ascites and capsular rupture.
Conclusion
Granulosa tumor is a rare tumor but you have to know how to think about an ovarian tumor.
It can occur at all ages, the juvenile form is the rarest, it constitutes a particular anatomopathological entity, it can be associated with other histological lesions such as glandulocystic hyperplasia of the uterus which can go up to degeneration.
Currently the treatment is based on surgery, whether it is an initial intervention or for recurrence.
- Ellouz S, Krichen-Makni S, Trabelsi K, Ayadi L, Sellami A, Khabir A. Laboratory of anatomy and pathological cytology chu Habib Bourguiba 3029 Sfax. Tunisia. 2006.
- Gittleman AM, Price AP, Coren C, Akhtar M, Donovan V, Katz DS. Juvenile granulosa cell tumor. Clin Imaging. 2003 Jul-Aug;27(4):221-4. doi: 10.1016/s0899-7071(02)00586-7. PMID: 12823914.
- Bompas E, Freyer G, Vitrey D, Trillet-Lenoir V. Tumeur à cellules de la granulosa: revue de la littérature [Granulosa cell tumour: review of the literature]. Bull Cancer. 2000 Oct;87(10):709-14. French. PMID: 11084534.
- Aitbouhou R, Kassimi I, Kessab A, Issa I, El Mangoub F, Moussaoui DR. Rare Malignant Tumor of the Ovarian: Mixed Ovarian Tumor Associated Mucinous Adenocarcinoma and Granulosa Tumor A Case Report. Global Academic Journal of Medical Sciences. 2019; 1: 29-32.
- Tavasoli FA, Mooney E, Gersell DJ. Sex cord stromal tumors. In Travasoli FA, Devilee P. Eds world health organization classification of tumors, pathology and genetics. lyon: 2011; 146-61.
- Savchenko O, Skorik V, Babii H, Savchenko P. Histological features and immunohistochemical diagnosis granulosa cell tumors. Ukraine : s.n., April 2021, Languages,Science and Practices.
- Sando Z, Mayeni ER, Bell E, Atangana PA, Mandeni Nikodo JM, Ndoumba A. granolosa cells tumors: a report of two cases anatomy and pathologies department of the Pasteur Center laboratories of Cameroon. Health Sci. 2015; 16.
- Elidrissi F, Ounejma S, Zeradi N, Barhmi RS, Fadli A, Achour M. Granulosa tumor of the ovary about a case. 1999; Medicine of the Maghreb. 76; 21-7.
- Hattman LC, Youg RH-Pordratz Kc. ovarien sex cord stromal tumors. In Hoskin WJ, Perez CA, Young RC (eds). Lippincott Williams. Principals and practice of gynecologic oncology. 2000; 36.
- Mouko A, Moukassa D, Leroy X, Ibara J, Makosso E, Bikandou G, Kalengayi RM, Senga P. Pseudo-puberté précoce isosexuelle révélatrice d'une tumeur de la granulosa juvénile chez une fillette congolaise de 3 ans [Early isosexual precocious pseudopuberty revealing a juvenile granulosa cell tumor in a 3-year-old Congolese girl]. Ann Pathol. 2000 May;20(3):245-8. French. PMID: 10891723.
- Kdous M, Hachicha R, Gamoudi A. Pseudo-puberté précoce isosexuelle révélant une tumeur de la granulosa juvénile chez une petite fille de six ans [Early isosexual precocious pseudopuberty revealing a juvenile granulosa cell tumor in a six-year-old girl]. Gynecol Obstet Fertil. 2004 Apr;32(4):311-4. French. doi: 10.1016/j.gyobfe.2004.02.009. PMID: 15123101.
- Sehouli J, Drescher FS, Mustea A, Elling D, Friedmann W, Kühn W, Nehmzow M, Opri F, Klare P, Dietel M, Lichtenegger W. Granulosa cell tumor of the ovary: 10 years follow-up data of 65 patients. Anticancer Res. 2004 Mar-Apr;24(2C):1223-9. PMID: 15154651.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
