Open Journal of Pediatrics and Child Health
Factors influencing the development and implementation of pediatrics in family-centered care model: A scoping review
Yue Ming Peng1,2, Yuan Shan2,3 and Xudong Yan1*
2Philippine Women’s University School of Nursing, 1743 Taft Ave, Malate, Manila, 1004 Metro Manila, Philippines
3Chengde Medical University, Chengde City, Hebei Province, China
Cite this as
Peng YM, Shan Y, Yan X (2024) Factors influencing the development and implementation of pediatrics in family-centered care model: A scoping review. Open J Pediatr Child Health 9(1): 033-039. DOI: 10.17352/ojpch.000055Copyright
© 2024 Peng YM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Introduction: Family-Centered Care (FCC) in neonatal healthcare emphasizes collaborative efforts between medical staff and families. This approach, rooted in mutual respect and active family participation, aims to enhance infant care outcomes. However, understanding the underlying forces behind FCC interventions remains challenging due to the diverse methods employed in healthcare practices.
Methods: We conducted a scoping review in June 2023. We searched Embase, Medline, CINAHL, Web of Science, Cochrane Library, Joanna Briggs Institute (JBI), PubMed, and PsycINFO. Inclusion criteria encompassed English language studies on Family-centered care and related factors, without date or geographic restrictions.
Results: Fifteen pertinent studies meeting the inclusion criteria were identified. Five pivotal components of modern FCC emerged: effective communication, active patient and family involvement, robust family support systems, organizational considerations, and the nurturing attitude of nurses.
Discussion: Family-centered care emerges as a comprehensive healthcare approach focusing on the interdependence of patients, healthcare professionals, and families. By recognizing this interconnection, FCC seeks to ensure the satisfaction and well-being of all stakeholders. Implementing FCC strategies presents challenges, emphasizing the need for continuous exploration and refinement.
Conclusion: Embracing family-centered care principles enriches patient-centered healthcare by involving families as active partners in the care process. Acknowledging the integral role of families enhances care quality and contributes to improved patient outcomes. Ongoing research and dialogue are essential for refining FCC models, ensuring successful implementation, and fostering patient-centered healthcare environments.
Introduction
Family-Centered Care (FCC) is a concept of care that relies on collaboration between the family and the medical staff to provide care to a newborn who is ill. The cooperative relationship is founded on decency and respect, information exchange, and the involvement of the family via their developed abilities to provide crucial infant care [1]. If they are not included in the care of unwell newborns, parents frequently report feeling distressed, frustrated, and alienated. However, if parents are given the chance to participate in treatment, receive honest updates on their newborn’s condition from medical professionals, and build relationships with those same professionals, they will feel satisfied and under less stress [2]. FCC implementation has been found to shorten preterm infants’ hospital stays, improve their health, enable more effective use of human resources, and promote parent-infant bonding. Particular FCC techniques, like as parent-provided kangaroo (skin-to-skin) care, boost weight growth, improve rates of effective breastfeeding, and prevent baby mortality and illness. Additionally, Kangaroo Mother Care (KMC) influences a newborn’s brain development by regulating heart rate, oxygenation, and sleep quality [3]. It is found to have long-term effects on IQ and attention among newborns born with neurological vulnerability [4]. Among other benefits, KMC reduces a baby’s stress and pain [5] while it may also have maternal benefits such as preventing postpartum depression [6]. In the first six months, mothers who gave KMC to their children showed signs of reduced anxiety and depression symptoms as well as more pleasant relationships with their offspring [7]. Infant massage increases alertness before and after feeding [8] and has been shown to contribute to daily weight gain and reduced length of stay [9]. Massaging infants is also seen to reduce maternal anxiety and depression [10]. When moms are present in the NICU, breastfeeding becomes feasible and frequent, which ultimately improves newborn health outcomes. Breastfeeding has been shown to boost IQ, prevent childhood illnesses and malocclusion, and reduce obesity and diabetes. Breastfeeding moms had a lower risk of diabetes, breast cancer, and ovarian cancer [11]. According to a randomized controlled experiment (RCT) in India, moms who participated in FCC for their unwell babies saw higher rates of breastfeeding than mothers in the control group, whose sick newborns got standard clinical treatment [12]. The difficulty is to pinpoint the driving forces behind these intervention measures because there are several implemented methods including FCC and related measures.
Methods
Eligibility criteria
Study design: For the purposes of this review, experimental studies, observational studies, descriptive designs, qualitative research, and gray literature were all taken into consideration.
Types of studies: The research on the variables affecting the adoption of the child-centered care approach by families or children. Implementation methods, risks, rewards, and finance models are just a few of the subjects the plan may address. The job health settings, such as community, emergency, home, or inpatient wards, including continuation services, can serve as the foundation for the focused care approach. Studies were disregarded if they weren’t written in English or didn’t include a comprehensive strategy for the center-of-care model’s results and procedures.
Search methods for inclusion of studies
Electronic searches: An initial scoping review was performed to identify gaps within the literature. A search of Medline and Google Scholar served to identify additional keywords for the search strategy. Terms related to, children, pediatrics (‘pediatrics∗’, ‘Pediatric Emergency Medicine’, ‘Pediatric Emergency’, ‘child∗’); terms related to centered care model∗’, ‘centered∗’, ‘care∗ , ‘framework∗’, ‘model∗’); and terms related to the family (‘Families∗’, ‘Family Member∗) were used to identify further key terms. We trialled the initial search strategy which included a search using terms related to advanced practice nursing. The first 3300 records returned were reviewed. ” Once all terms were agreed upon by all authors, concepts were combined with Boolean operators ‘AND’ and ‘OR’. A three-step search process was implemented. The initial studies were identified through a systematic search of eight electronic databases (Embase, Medline, CINAHL, Web of Science, Cochrane Library, Joanna Briggs Institute (JBI), PubMed, and PsycINFO) in June 2023. A hand search was conducted from reference lists of published systematic reviews and relevant topical papers. A gray literature search strategy, was used to complement the research literature, and was framed by key stages: involved a review of gray literature websites with a focus placed on children or family members with family-centered care model frameworks; no timeframe parameters were used. Title screening was performed by two independent reviewers within Endnote X9. The abstract screening was then completed independently by two reviewers. Studies were deemed appropriate for a full-text analysis if the a priori eligibility criteria were addressed. Full-text screening was undertaken by three independent reviewers.
Data extraction
Three separate research members independently retrieved data from pertinent papers using a modified version of the JBI standard data extraction tool (Joanna Briggs Institute 2017). Data retrieved addressed the following topics: nation, research design, sample size, demographics of the sample, setting, program type (specific to the profession), data collection techniques, and information on the subjects covered by programs or models.
Data synthesis
Data extracted from each study were narratively synthesised by three independent research members. Study characteristics of the included literature are displayed in Table 1.
Results
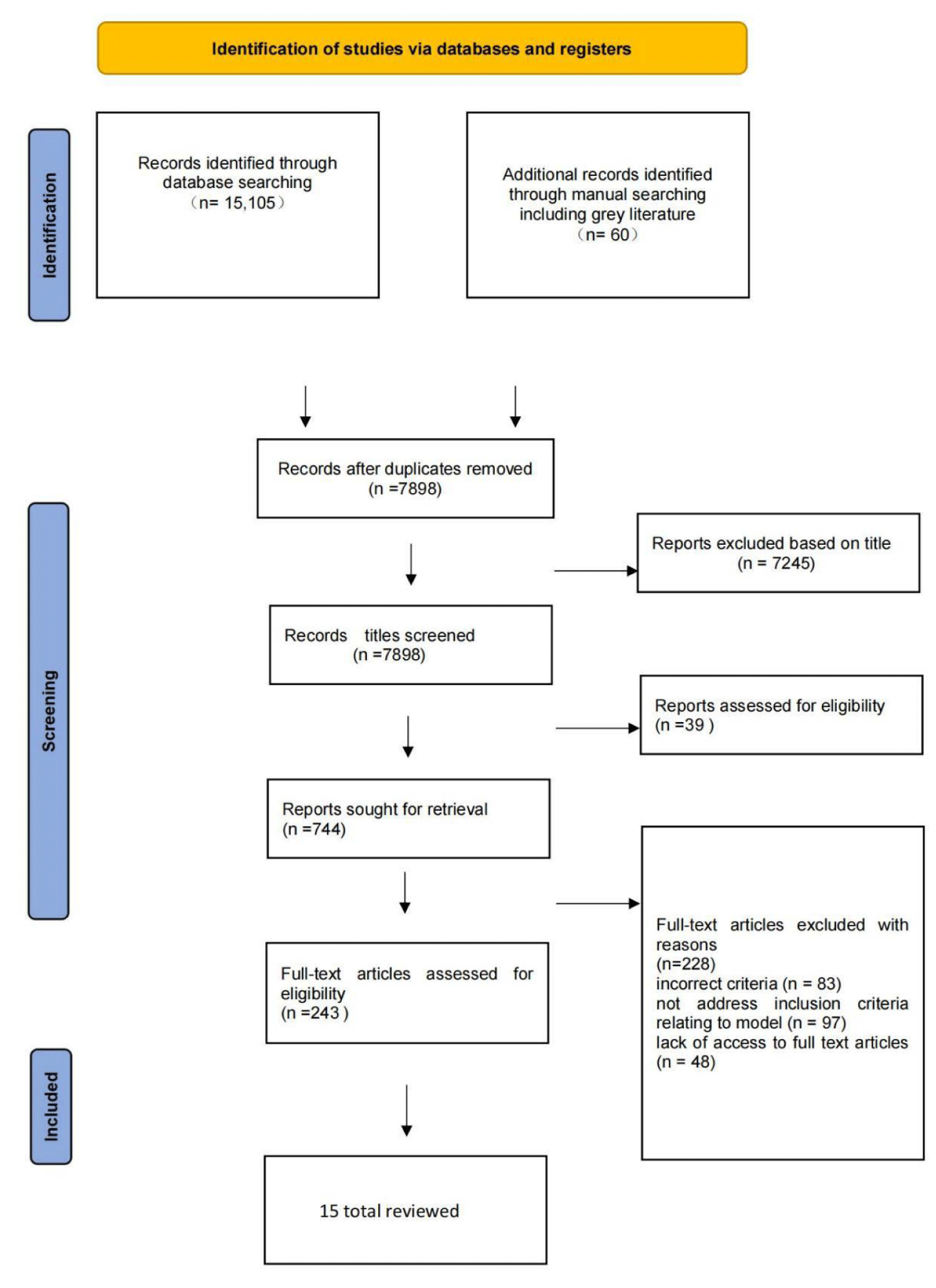
A total of 15,165 references were retrieved. After duplicates were removed, a total of 5,980 references remained for title screening. Of these, 744 titles were accepted by both reviewers, and abstracts were assessed, with 243 abstracts meeting the eligibility criteria. A further 198 items were excluded at the full-text review as not meeting the inclusion criteria. Reasons for exclusion included incorrect criteria (n = 83), did not address inclusion criteria relating to the model (n = 97), and lack of access to full-text articles (n = 48). A total of 15 peer-reviewed articles were included in the database review (Figure 1).
For modern family-centered care, these components are essential. Five crucial elements of family-centered care have been discovered: communication; involvement of patients and family members; support to family members; organizational aspects and suggestions and attitude of nurses.
Communication
Any intersubjective reality must include communication as one of its distinguishing features. The necessity of appropriate and accurate information exchange in family-centered care was underlined in a number of the studies that we evaluated for this study. This was accomplished by either highlighting the benefits of effective communication [13-17].
Poor health literacy among patients and family members is one reason for disconnected communication, which frequently greatly reduces their involvement and participation in care [15]. The importance of education in relation to the post-hospitalization phase is thus emphasized by some authors [17], as well as the importance of education regarding care provision and disease [14]. It is important to provide information in a way that will help patients and their families grasp it [15].
On the other hand, healthcare professionals frequently disregard patients’ and family members’ low levels of health literacy [15]. Some authors emphasized the significance of healthcare provider education and training [13,16] because it facilitates communication, equips professionals to work with patients and family members who have varying levels of health literacy, and enables them to identify the needs and shortfalls of patients and their families [18]. Nurses spend the most time providing direct patient care of any medical professional, thus it’s critical that they communicate well [15]. Communication is always two-sided, thus it’s important for medical professionals to have a grasp of their patients’ conditions through the distinct and specialized knowledge that only patients and their families can offer [15].
Involvement of patients and family members
The active involvement of the patient and family members in the medical process is one of the distinguishing traits of family-centered care. The publications we used for our study referred to patient and family involvement in medical procedures using the following two terms: involvement [19-21] and participation [13,16-17,22].
These two concepts are linked and were frequently used in the same sentence. Patient and family participation occurs when the opinions and experiences of patients and families are sought out and taken into consideration in healthcare, according to Whiston, Barry, O’Keane, and Darker [22]. The notion of patient involvement stems from the tenet that patients should receive comprehensive care [21] and is consequently inextricably linked to the idea of family-centered care, which emphasizes the significance of the intersubjective unit of care made up of a patient, family members, and healthcare professionals. There are several ways that patients and family members can participate in the medical procedure.
They are able to take part in important caregiving activities, information exchange, and cooperative decision-making [16]. Global consensus has been reached about the significance of patient involvement in healthcare [22]. It increases patient, family, and healthcare provider satisfaction [20], improves healthcare process outcomes [19] and aids in preserving patient and family control over care delivery [14].
The beneficial impact that family members may have on the patient is another crucial component of family engagement in health care procedures [15]. However, healthcare professionals occasionally voice their reluctance to include family members in the healthcare process [23]. According to Mitchell, Chaboyer, Burmeister, and Foster [18,21], the intricacy of their job may be the root of these scruples, while other scholars have noted that lack of experience and education may also be to blame [23].
Support to family members
The support given to family members and patients is another feature of family-centered care that was frequently emphasized by the authors [14,16-17]. Family members and patients can receive a variety of types of assistance, including practical, emotional, and social support (which aims to improve social skills) [18].
Physical assistance is a crucial component of family-centered care [16]. Family members may have detrimental effects on their own well-being, hence it is critical that models of family-centered care are supportive of them in such circumstances [14]. According to Petry, Ernst, Seinbrüchel-Boesch, Altherr, & Naef [17], engaging family members in the healthcare process inherently boosts family members’ happiness. However, due to their ambiguous knowledge of the viewpoints of the patients, several investigators discovered potential harmful effects of the family members’ support [24].
Organizational aspects and suggestions
Any network of connected variables is greater than the sum of its parts. This premise serves as the foundation for the idea of family-centered care. So, in the context of family-centered care, a number of authors emphasized the significance of organizational solutions. In actuality, this implies that rules should be put in place that would encourage family-centered care [13]. Typically, writers recommended that institutions that offer healthcare also adopt rules that would take into account the needs and desires of its staff, patients, and families [13,14]. The authors suggested initiatives to improve the communication abilities of healthcare professionals [13]. Encouragement of family and patient involvement in health care was another crucial component of the suggested policy [18]. Such policies ought to address several facets of family-centered care, including family support, communication, operational challenges, and environmental concerns [13].
Attitudes of nurses
One of the aspects emphasized by the authors is the connection between healthcare practitioners’ willingness or capacity to include patients and family members and the standard of treatment [23]. The way nurses view their function in the family is likely to have an impact on the encounter’s quality. While negative attitudes cause nurses to minimize family participation, good attitudes are necessary for welcoming and including families in nursing care [25].
An assessment tool for nurses’ views on the significance of families in nursing care was developed by Luttik et al., Benzein et al. [23,26] and Gusdal, Josefsson, Adolfsson, & Martin both employed this instrument further [25]. Because they spend the most time with patients and their families, nurses have a vital role in the delivery of healthcare [14]. In general, nurses advocate family engagement and concur that having family members there is crucial [23,25]. However, findings from both research indicated that opinions regarding including family members in the patient’s treatment were less favorable [23,25]. The opinions of older, more seasoned nurses and younger, less educated nurses seemed to diverge. Nurses with higher education and experience were more supportive of family engagement [23,25]. Both of the research emphasized that younger nurses are more attentive to specific patients and preoccupied with their own learning while attempting to explain the causes of this trend [23,25]. They feel as though they are being examined while the family is there, which adds to their stress [23]. Both studies [23,25] emphasized the value of education on the role of families and active family engagement in patient treatment, and both called for an organizational-level solution. Gusdal, Josefsson, Adolfsson, & Martin [25] proposed encouraging older, more seasoned nurses to mentor and coach their younger, less seasoned coworkers in order to improve the latter’s supportive views toward families [28].
Discussion
When doing our evaluation, we looked for five key aspects of family-centered care that were emphasized in the publications. These include the significance of communication, family and member engagement, support for family members, organizational factors and recommendations, and nursing attitudes regarding family involvement. We can infer some implications from the aforementioned findings and recommendations. The first is that effective and efficient healthcare depends on positive relationships between patients, their families, and medical professionals. From our concept of family-centered care as an intersubjective reality, it is already possible to draw this conclusion. The importance of relationships between parties involved, which elevate the system as a whole above the mere sum of its parts, is particularly evident in the inter-subject of family-centered care. It has been emphasized several times that proper relationships in some way affect everyone’s enjoyment. This is why several authors emphasized the value of effective communication, which enables patients, families, and healthcare professionals to effectively convey their needs, opinions, and requests.
Another significant factor that commonly occurred in the publications under evaluation was the involvement of patients and family members at different stages of the healthcare process [29]. As a result, it is founded on one of the fundamental tenets of family-centered care, which holds that because patients and families make up a unit of care, it is essential that they participate in some way in the delivery of healthcare. Family engagement is also founded on the idea that patient and family expertise may be particularly valuable to the success of the healthcare process when family-centered treatment is provided. Parents may have stronger beliefs about their parental role when having the opportunity to accompany their baby and be empowered by medical staffs [27]. So, including family members enhances healthcare outcomes while also boosting satisfaction among patients, healthcare professionals, and family members. Family members’ need for assistance depends on effective communication and relationships. The ability of healthcare professionals to accurately assess health literacy and other competencies of family members and patients is crucial in providing help to families [30].
The necessity for organizational solutions to the problems observed was mentioned in almost all of the articles reviewed. This method is also predicated on the idea that problems may be effectively addressed and solved by forging good relationships. Organizational solutions go beyond the capabilities of each party that is involved and place those parties in a way that maximizes happiness for all parties [31]. Because they take into account all parties involved, organizational solutions are essential for family-centered care. A frequent example of the necessity for organizational solutions is the requirement for regulations that would organize various components of family-centered care. Because of this, organizational solutions are able to consider the happiness of all parties and do not focus just on one.
Nurses are among the healthcare professionals who maintain regular contact with patients and their families. The ability of nurses to build strong relationships with patients and family members is essential for providing family-centered care since only in this way can patients and family members experience better levels of satisfaction [32]. Because it evaluates nurses’ views regarding family participation and identifies factors that impact such attitudes, the instrument created by Benzein, Johansson, Restedt, Berg, and Saveman [26] is crucial in this field.
The effectiveness of healthcare suffers when nurses have a bad attitude towards involving family members in the healing process. This fact can be understood in light of the intersubjective nature of all medical procedures. The degree of ultimate efficacy and of everyone’s happiness is reduced when proper relationships are somehow harmed and are not established [33]. Since only then can we address them and strive to overcome them with a methodical solution that takes into account all involved parties, it is crucial to understand the causes of unfavorable attitudes toward including family members in the healthcare process.
Conclusion
Family-centered care is a healthcare delivery strategy that seeks to improve results by taking into account all stakeholders involved in the delivery of care. Its fundamental belief is that because patients, healthcare professionals, and family members are all components of a system, their pleasure is interdependent. Family-centered care offers a methodical strategy that considers all the parties involved in order to maximize everyone’s pleasure. Proper and accurate communication, which is a fundamental dynamic of every inter-subjective reality, is essential to this solution. Numerous issues that influence communication should be addressed by effective policies. The attitudes of nurses toward involving family members in healthcare operations are a crucial component of family-centered care.
Funding
The study was partially supported by the Shenzhen Science and Technology Program (Grant No.JCYJ20210324114213037).
- Ahmann E, Abraham MR, Johnson BH. Changing the Concept of Families as Visitors: Supporting Family Presence and Participation. Bethesda, MD: Institute for Family-centered Care. 2003.
- Obeidat HM, Bond EA, Callister LC. The parental experience of having an infant in the newborn intensive care unit. J Perinat Educ. 2009 Summer;18(3):23-9. doi: 10.1624/105812409X461199. PMID: 20514124; PMCID: PMC2730907.
- Schneider C, Charpak N, Ruiz-Peláez JG, Tessier R. Cerebral motor function in very premature-at-birth adolescents: a brain stimulation exploration of kangaroo mother care effects. Acta Paediatr. 2012 Oct;101(10):1045-53. doi: 10.1111/j.1651-2227.2012.02770.x. Epub 2012 Jul 17. PMID: 22734793.
- Ropars S, Tessier R, Charpak N, Uriza LF. The long-term effects of the Kangaroo Mother Care intervention on cognitive functioning: Results from a longitudinal study. Dev Neuropsychol. 2018 Jan;43(1):82-91. doi: 10.1080/87565641.2017.1422507. PMID: 29377735.
- Ludington-Hoe SM, Hosseini R, Torowicz DL. Skin-to-skin contact (Kangaroo Care) analgesia for preterm infant heel stick. AACN Clin Issues. 2005 Jul-Sep;16(3):373-87. doi: 10.1097/00044067-200507000-00010. PMID: 16082239; PMCID: PMC1890009.
- Dombrowski MA, Anderson GC, Santori C, Burkhammer M. Kangaroo (skin-to-skin) care with a postpartum woman who felt depressed. MCN Am J Matern Child Nurs. 2001 Jul-Aug;26(4):214-6. doi: 10.1097/00005721-200107000-00012. PMID: 11452667.
- de Macedo EC, Cruvinel F, Lukasova K, D'Antino ME. The mood variation in mothers of preterm infants in Kangaroo mother care and conventional incubator care. J Trop Pediatr. 2007 Oct;53(5):344-6. doi: 10.1093/tropej/fmm076. Epub 2007 Sep 19. PMID: 17881409.
- White-Traut RC, Schwertz D, McFarlin B, Kogan J. Salivary cortisol and behavioral state responses of healthy newborn infants to tactile-only and multisensory interventions. J Obstet Gynecol Neonatal Nurs. 2009 Jan-Feb;38(1):22-34. doi: 10.1111/j.1552-6909.2008.00307.x. PMID: 19208045.
- Vickers A, Ohlsson A, Lacy JB, Horsley A. Massage for promoting growth and development of preterm and/or low birth-weight infants. Cochrane Database Syst Rev. 2004;2004(2):CD000390. doi: 10.1002/14651858.CD000390.pub2. PMID: 15106151; PMCID: PMC6956667.
- Feijó L, Hernandez-Reif M, Field T, Burns W, Valley-Gray S, Simco E. Mothers' depressed mood and anxiety levels are reduced after massaging their preterm infants. Infant Behav Dev. 2006 Jul;29(3):476-80. doi: 10.1016/j.infbeh.2006.02.003. Epub 2006 Mar 27. PMID: 17138300.
- Victora CG, Bahl R, Barros AJ, França GV, Horton S, Krasevec J, Murch S, Sankar MJ, Walker N, Rollins NC; Lancet Breastfeeding Series Group. Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. Lancet. 2016 Jan 30;387(10017):475-90. doi: 10.1016/S0140-6736(15)01024-7. PMID: 26869575.
- Verma A, Maria A, Pandey RM, Hans C, Verma A, Sherwani F. Family-Centered Care to Complement Care of Sick Newborns: A Randomized Controlled Trial. Indian Pediatr. 2017 Jun 15;54(6):455-459. doi: 10.1007/s13312-017-1047-9. PMID: 28667715.
- Davidson JE, Aslakson RA, Long AC, Puntillo KA, Kross EK, Hart J, Cox CE, Wunsch H, Wickline MA, Nunnally ME, Netzer G, Kentish-Barnes N, Sprung CL, Hartog CS, Coombs M, Gerritsen RT, Hopkins RO, Franck LS, Skrobik Y, Kon AA, Scruth EA, Harvey MA, Lewis-Newby M, White DB, Swoboda SM, Cooke CR, Levy MM, Azoulay E, Curtis JR. Guidelines for Family-Centered Care in the Neonatal, Pediatric, and Adult ICU. Crit Care Med. 2017 Jan;45(1):103-128. doi: 10.1097/CCM.0000000000002169. PMID: 27984278.
- Kokorelias KM, Gignac MAM, Naglie G, Cameron JI. Towards a universal model of family centered care: a scoping review. BMC Health Serv Res. 2019 Aug 13;19(1):564. doi: 10.1186/s12913-019-4394-5. PMID: 31409347; PMCID: PMC6693264.
- Mitchell M, Chaboyer W, Burmeister E, Foster M. Positive effects of a nursing intervention on family-centered care in adult critical care. Am J Crit Care. 2009 Nov;18(6):543-52; quiz 553. doi: 10.4037/ajcc2009226. PMID: 19880956.
- Park M, Giap TT, Lee M, Jeong H, Jeong M, Go Y. Patient- and family-centered care interventions for improving the quality of health care: A review of systematic reviews. Int J Nurs Stud. 2018 Nov;87:69-83. doi: 10.1016/j.ijnurstu.2018.07.006. Epub 2018 Jul 26. PMID: 30056169.
- Petry H, Ernst J, Steinbrüchel-Boesch C, Altherr J, Naef R. The acute care experience of older persons with cognitive impairment and their families: A qualitative study. Int J Nurs Stud. 2019 Aug;96:44-52. doi: 10.1016/j.ijnurstu.2018.11.008. Epub 2018 Dec 31. PMID: 30660445.
- Foster K, Maybery D, Reupert A, Gladstone B, Grant A, Ruud T, Falkov A. Family-focused practice in mental health care: An integrative review. Child Youth Serv. 2016; 37(2):129-155. doi: 10.1080/0145935X.2016.1104048.
- Deek H, Hamilton S, Brown N, Inglis SC, Digiacomo M, Newton PJ, Noureddine S, MacDonald PS, Davidson PM; FAMILY Project Investigators. Family-centred approaches to healthcare interventions in chronic diseases in adults: a quantitative systematic review. J Adv Nurs. 2016 May;72(5):968-79. doi: 10.1111/jan.12885. Epub 2016 Jan 10. PMID: 26751971.
- Hertel E, Cheadle A, Matthys J, Coleman K, Gray M, Robbins M, Tufte J, Hsu C. Engaging patients in primary care design: An evaluation of a novel approach to codesigning care. Health Expect. 2019 Aug;22(4):609-616. doi: 10.1111/hex.12909. Epub 2019 May 27. PMID: 31134725; PMCID: PMC6737754.
- Mackie BR, Mitchell M, Marshall AP. Patient and family members' perceptions of family participation in care on acute care wards. Scand J Caring Sci. 2019 Jun;33(2):359-370. doi: 10.1111/scs.12631. Epub 2018 Dec 3. PMID: 30507038.
- Whiston L, Barry J, O’Keane V, Darker C. Patient, family and clinician preferences for the intensity and implementation of patient and family participation in healthcare design and delivery in psychiatry. Eur J Psychiatry. 2018; 33(1):8-16. doi: 10.1016/j.ejpsy.2018.07.001.
- Luttik M, Goossens E, Ågren S, Jaarsma T, Mårtensson J, Thompson DR, Moons P, Strömberg A; Undertaking Nursing Interventions Throughout Europe (UNITE) research group. Attitudes of nurses towards family involvement in the care for patients with cardiovascular diseases. Eur J Cardiovasc Nurs. 2017 Apr;16(4):299-308. doi: 10.1177/1474515116663143. Epub 2016 Jul 29. PMID: 27470053.
- Wolff JL, Guan Y, Boyd CM, Vick J, Amjad H, Roth DL, Gitlin LN, Roter DL. Examining the context and helpfulness of family companion contributions to older adults' primary care visits. Patient Educ Couns. 2017 Mar;100(3):487-494. doi: 10.1016/j.pec.2016.10.022. Epub 2016 Oct 25. PMID: 27817986; PMCID: PMC5350029.
- Gusdal AK, Josefsson K, Thors Adolfsson E, Martin L. Nurses' attitudes toward family importance in heart failure care. Eur J Cardiovasc Nurs. 2017 Mar;16(3):256-266. doi: 10.1177/1474515116687178. Epub 2017 Jan 4. PMID: 28051331.
- Benzein E, Johansson P, Arestedt KF, Berg A, Saveman BI. Families' Importance in Nursing Care: Nurses' Attitudes--an instrument development. J Fam Nurs. 2008 Feb;14(1):97-117. doi: 10.1177/1074840707312716. PMID: 18281645.
- Melnyk BM, Feinstein NF, Alpert-Gillis L, Fairbanks E, Crean HF, Sinkin RA, Stone PW, Small L, Tu X, Gross SJ. Reducing premature infants' length of stay and improving parents' mental health outcomes with the Creating Opportunities for Parent Empowerment (COPE) neonatal intensive care unit program: a randomized, controlled trial. Pediatrics. 2006 Nov;118(5):e1414-27. doi: 10.1542/peds.2005-2580. Epub 2006 Oct 16. PMID: 17043133.
- Neu M, Robinson J. Maternal holding of preterm infants during the early weeks after birth and dyad interaction at six months. J Obstet Gynecol Neonatal Nurs. 2010 Jul-Aug;39(4):401-14. doi: 10.1111/j.1552-6909.2010.01152.x. PMID: 20629927; PMCID: PMC2935695.
- Hsu C, Gray MF, Murray L, Abraham M, Nickel W, Sweeney JM, Frosch DL, Mroz TM, Ehrlich K, Johnson B, Reid RJ. Actions and processes that patients, family members, and physicians associate with patient- and family-centered care. BMC Fam Pract. 2019 Feb 25;20(1):35. doi: 10.1186/s12875-019-0918-7. PMID: 30803446; PMCID: PMC6388493.
- Johnson BH. Family-centered care: Four decades of progress. Fam Syst Health. 2000; 18(2):137-156. doi: 10.1037/h0091843.
- Jolley J, Shields L. The evolution of family-centered care. J Pediatr Nurs. 2009 Apr;24(2):164-70. doi: 10.1016/j.pedn.2008.03.010. Epub 2008 Oct 18. PMID: 19268238.
- Kovacs PJ, Bellin MH, Fauri DP. Family-Centered Care. J Soc Work End Life Palliat Care. 2008; 2(1):13–27. doi: 10.1300/J457v02n01_03.
- Robertson J, Bowlby J. Responses of young children to separation from their mothers. Courrier Centre International de l'enfance. 1952; 2:131-142.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
