Open Journal of Pediatrics and Child Health
Trivial trauma as a cause of stroke in children
Clara Rilna Joseph, K Shreedhara Avabratha*, Rashmi Alva and Raghavendra BS#
Cite this as
Joseph CR, Avabratha KS, Alva R, Raghavendra BS (2020) Trivial trauma as a cause of stroke in children. Open J Pediatr Child Health 5(1): 001-002. DOI: 10.17352/ojpch.000021Ischaemic stroke resulting from minor head injury are rare in children, as trauma usually results in intracranial bleed. We report a case who presented with right sided hemiplegic stroke due to trivial trauma. 11 year old girl who was previously healthy, presented with right sided facial palsy and ipsilateral hemiplegia of one day. MRI brain showed left sided middle cerebral artery territory infarct. MR angiography showed left middle cerebral artery territory infarct involving the left gangliocapsular region, left corona radiata and left frontotemporal lobe, suggestive of occlusion. On enquiry mother revealed fall from stairs 3 days back.
Introduction
Stroke is defined as a clinical syndrome of rapidly developing focal or global disturbance of cerebral function lasting more than 24hours or leading to death with no apparent non-vascular aetiology [1]. The major risk factors in children include cardiac diseases like cardiomyopathies, rheumatic heart disease, endocarditis, haematological causes like sickle cell anaemia, prothrombotic disorders secondary to protein C and S deficiencies, leukaemia, lymphoma, post infectious–varicella infection, HIV infection, vascular causes like arteriovenous malformations, Moyamoya, drugs like cocaine, ecstasy, head and neck trauma resulting in dissection of carotid or vertebral arteries1. Ischaemic stroke resulting from minor head injury is rare in children [2], as trauma usually results in intracranial bleed. We report a case who presented with right sided hemiplegic stroke due to trivial trauma.
Case report
An 11-year-old girl, who was previously healthy, presented with weakness of right upper and lower limbs, deviation of face to left with slurring of speech of one day. There was no history of fever, seizures, ear discharge, rashes, respiratory illness, photophobia or mucocutaneous bleed. Child was disoriented at the time of admission. She was afebrile, with a blood pressure of 108/70mmHg. Central nervous system examination revealed right sided facial paralysis, no signs of papilloedema and power of 2/5 in the right upper and lower limbs. Deep tendon reflexes were exaggerated on the right side. Meningeal signs were absent. No bruit was audible over the cranium or carotid artery.
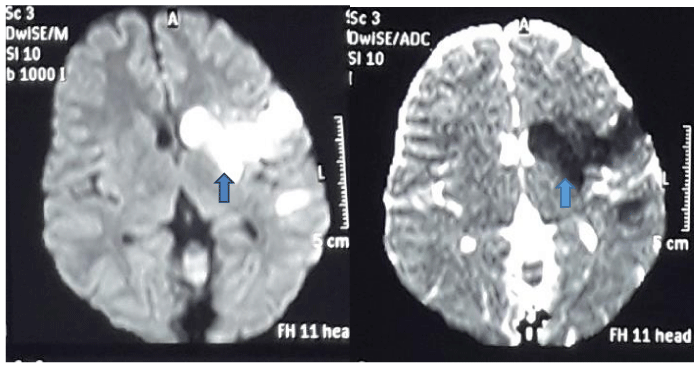
Computed Tomography (CT) scan was normal. Magnetic Resonance Imaging (MRI) of the brain showed left sided middle cerebral artery territory infarct (Figure 1).
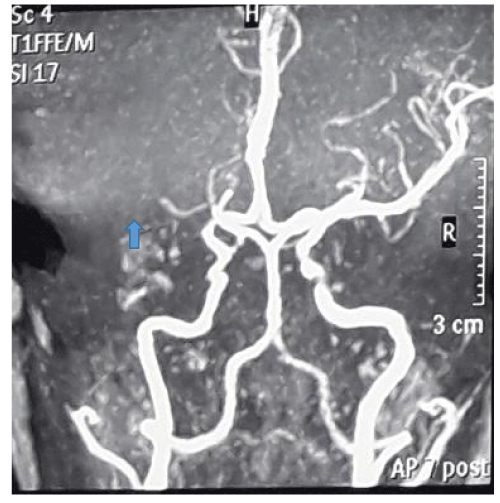
Magnetic resonance angiography showed left middle cerebral artery territory infarct involving the left ganglio-capsular region, left corona radiata and left frontotemporal lobe, suggestive of occlusion in the left middle cerebral artery (Figure 2).
Blood investigations revealed a normocytic, normochromic blood picture with neutrophilia. Liver and renal function as well as lipid profile were within normal range.Coagulation profile was normal. Protein C, protein S and homocysteine were within normal limits. Antinuclear antibody profile was negative. Echocardiography was normal. On enquiry, mother revealed history of trauma as the child had fallen down the stairs 3days back. She had not revealed that earlier as there was no external injury or loss of consciousness, hence considering it as insignificant. With other causes being ruled out, child’s stroke was attributed to this trivial trauma.
Child was treated with Low Molecular Weight Heparin (LMWH) for 10 days and discharged on aspirin and atorvastatin for 6months. Facial palsy and hemiparesis improved with 6-7days of treatment. On follow up, she showed complete clinical resolution.
Discussion
Stroke is relatively rare in the paediatric age group, the incidence in children ranging from 1.2 to 13 cases per 100,000 children [2]. In the study by Hilton-Jones et al 22% of cerebral infarcts in youth were traumatic in origin [3]. In a study by Kieslich M, et al., neurological manifestations developed 15minutes to 72hours following trauma [4]. Hemiplegia occurs in 94% of stroke cases [5]. Hyperextension or rotational injuries during trivial head trauma, car accidents and sports can also result in stroke [2].
Carotid artery spasm in the cervical region may cause post traumatic occlusion of intracranial arteries [5]. Thrombus formation may be due to direct trauma to the vessel wall, circulatory stasis or effects on the constitution of the circulating blood [4,6,7]. CT scan does not show a parenchymal infarct reliably within 24hours of an ischaemic stroke [8]. However, non contrast CT may help in excluding haemorrhagic stroke and may even reveal venous sinus thrombosis and occasionally other vascular abnormalities [9]. MRI is mandatory even if CT is normal. MRI with diffusion weighted imaging is considered the gold standard for ischaemic stroke in infants and children. MR angiography is a reasonable alternative to conventional arteriography. Imaging of extracranial circulations such as cervical MRA or Doppler ultrasound is important, especially if history is suggestive of cervical dissection [1,10].
Management of stroke involves supportive measures like reducing the increased intracranial pressure. Treatment measures should be taken to prevent further ischaemic events. Treatment schedule usually includes anticoagulation with low molecular weight heparin (LMWH) or unfractionated heparin. Haemorrhagic stroke needs to be excluded before starting treatment with LMWH [11]. Use of LMWH is controversial and recent studies have shown that there is no significant reduction in mortality or morbidity with the use of LMWH as compared to aspirin with clopidogrel combination [12]. Anti-platelets are reasonable for secondary stroke prevention. The Royal College of Physicians, International Paediatric Stroke study group recommends that thrombolysis should not be used in the treatment of paediatric stroke [1].
Conclusion
Stroke is relatively rare in children. The risk factors and clinical presentations are different as compared to adults. All possibilities should be kept in mind while dealing with paediatric stroke. A detailed history and thorough evaluation helps in proper diagnosis and management.
- Ciccone S, Cappella M, Borgna-Pignatti C (2011) Ischaemic stroke in infants and children: Practical management in emergency. Stroke Res Treat 2011: 736965. Link: http://bit.ly/38YluoR
- Tsze DS, Valente JH (2011) Paediatric Stroke: A Review. Emerg Med Int 2011: 734506. Link: http://bit.ly/2Og4PFe
- Jones DH, Warlow CP (1985) The causes of stroke in the young. J Neurol 232: 137-143. Link: http://bit.ly/2uOlzg5
- Kieslich M, Fiedler A, Heller C, Kreuz W, Jacobi G (2002) Minor head injury as cause and co-factor in the aetiology of stroke in childhood: a report of eight cases. J Neurol Neurosurg Psychiatry 73: 13-16. Link: http://bit.ly/2tjFALd
- Balachandran A, Kalyanshettar S, Patil S, Shegji V (2016) Ischaemic stroke in confederation with trivial head trauma. Case Rep Pediatr 2016: 2572958. Link: http://bit.ly/2vAT065
- Landi A, Marotta N, Mancarella C, Marruzzo D, Salvati M, et al. (2011) Basal ganglia stroke due to mild head trauma in paediatric age - clinical and therapeutic management: a case report and 10 year literature review. Ital J Pediatr 37: 2. Link: http://bit.ly/36M8t03
- Shaffer L, Rich PM, Pohl KRE, Ganesan V (2003) Can mild head injury cause ischaemic stroke? Arch Dis Child 88: 267-269. Link: http://bit.ly/37IpPMJ
- Kirkham F (2010) Investigation and management of childhood stroke. Paediatr Child Health 20: 428-438. Link: http://bit.ly/2SeyUGK
- Akinci E, Yuzbasioglu Y, Coskun F (2011) Post Traumatic Paediatric Ischaemic Stroke: Case Presentation. Hong Kong J Emerg Med 18: 169-172. Link: http://bit.ly/2S98TID
- Hollin S, Sukoff M, Silverstein A, Gross S (1966) Post-traumatic middle cerebral artery occlusion. J Neurosurg 25: 526-535. Link: http://bit.ly/36FKekg
- Rosa M, De Lucia S, Rinaldi V, Le Gal J, Desmarest M, et al. (2015) Paediatric arterial ischaemic stroke: acute management, recent advances and remaining issues. Ital J Pediatr 41: 95. Link: http://bit.ly/2RQ2uU1
- Singh K (2017) Current role of low molecular weight heparin in the treatment of acute ischaemic stroke. Int J Adv Med 4: 1599-1604. Link: http://bit.ly/31mf1Sc
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
